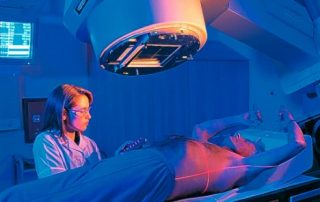
Why won’t our doctors face up to the dangers of radiotherapy?
Source: http://www.dailymail.co.uk/health/article-1089091/Why-wont-doctors-face-dangers-radiotherapy.html Author: Isla Whitcroft It's a life-saver for thousands - but the side-effects can be devastating. A year after he'd undergone treatment for cancer of the tonsils, Richard Wayman felt a painful tingling in his legs. Within weeks, the 59-year- old shopkeeper was struggling to walk. He was admitted to hospital, where doctors carried out scans, X-rays and tests. 'The scans revealed lesions on my lungs, which raised fears that the cancer had spread, so I was admitted to another hospital for a biopsy and, as a result, contracted MRSA and pneumonia,' recalls Richard, from Colchester in Essex. 'From 11-and-a-half stone I went down to eight-and-a-half stone. I thought I was never going to get out of there.' Finally, the lung lesions were diagnosed as a side-effect of the radiotherapy Richard had undergone for his cancer. However, his problems only got worse: a few weeks after a routine tooth extraction, the bone around the extraction started to crumble and become infected. Within months he had an open weeping wound, running from his lower cheek through his jaw and into his mouth. The diagnosis: bone necrosis as a direct result of radiotherapy damage to the jaw. Richard is one of the many thousands of cancer survivors who have developed terrible conditions as a result of the radiotherapy treatment that helped save them. Around 4 to 5 per cent of all head and neck cancer patients suffer problems with swallowing or breathing, fistulas (open holes) in the jaw and gum, loss [...]