Source: http://www.dailymail.co.uk/health/article-1089091/Why-wont-doctors-face-dangers-radiotherapy.html
Author: Isla Whitcroft
It’s a life-saver for thousands – but the side-effects can be devastating.
A year after he’d undergone treatment for cancer of the tonsils, Richard Wayman felt a painful tingling in his legs. Within weeks, the 59-year- old shopkeeper was struggling to walk. He was admitted to hospital, where doctors carried out scans, X-rays and tests.
‘The scans revealed lesions on my lungs, which raised fears that the cancer had spread, so I was admitted to another hospital for a biopsy and, as a result, contracted MRSA and pneumonia,’ recalls Richard, from Colchester in Essex.
‘From 11-and-a-half stone I went down to eight-and-a-half stone. I thought I was never going to get out of there.’
Finally, the lung lesions were diagnosed as a side-effect of the radiotherapy Richard had undergone for his cancer. However, his problems only got worse: a few weeks after a routine tooth extraction, the bone around the extraction started to crumble and become infected.
Within months he had an open weeping wound, running from his lower cheek through his jaw and into his mouth. The diagnosis: bone necrosis as a direct result of radiotherapy damage to the jaw.
Richard is one of the many thousands of cancer survivors who have developed terrible conditions as a result of the radiotherapy treatment that helped save them.
Around 4 to 5 per cent of all head and neck cancer patients suffer problems with swallowing or breathing, fistulas (open holes) in the jaw and gum, loss of taste and hearing.
But the problem is not unique to these cancers. Up to 10 per cent of breast cancer patients suffer radiation damage to their heart, lungs or the nerves to the arms (leading to loss of circulation and movement).
Every year, another 6,000 patients who’ve had pelvic radiotherapy treatment for conditions such as bowel cancer suffer long-term damage (including incontinence). A thousand of these patients go on to suffer even worse problems, such as intestinal failure or heavy bleeding.
It is clear that radiation damage is a significant health care issue. Yet, to date, there has been no national attempt to collate statistics that would enable any significant research work to begin.
Remarkably, it is not even officially classified as a specific medical condition; nor is there any definitive information on how to deal with it.
As a result, when it comes to treating the problems, patients can be offered a mix of options. Some are treated by a urologist, others are referred to a gastroenterologist, or an ear, nose and throat expert, while women often see a gynaecologist. This means many people will go undiagnosed for months and often years.
‘Until recently, radiotherapy damage has not been a priority in the treatment of cancer,’ says oncologist Paul Cornes, who runs clinics for patients with radiotherapy damage.
‘It is not a deliberate cover up; but in the past, cancer medicine was all about the treatment and giving patients a chance of life. Now we must address quality of life after cancer.’
Dr Sylvie Delanian, a radiologist and oncologist at the Hospital St Louis in Paris, is one of the few radiologists around the world to research and treat the condition. ‘Long-term radiotherapy damage is a taboo subject,’ she argues.
‘Radiologists are often frightened to discuss the matter with patients in case they refuse treatment. There is also the feeling that “we’ve saved your life, now go away and live with the side-effects”.’
Indeed, some hospitals seem to actively discourage discussion about the subject. While we were investigating this article, one London trust refused to allow Good Health to speak to their specialist, while another major cancer centre barred us from a conference on pelvic radiotherapy damage.
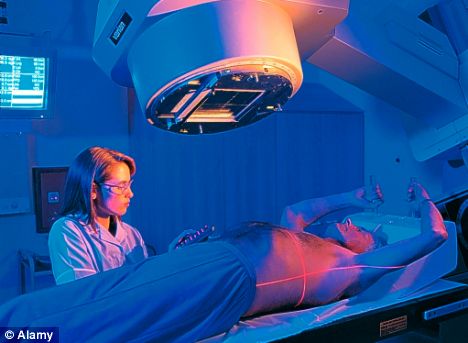
Radiotherapy is an incredibly successful method of treating cancer, increasing survival rates by around 50 per cent. It works by bombarding the tumour or tumour site with X-rays to kill the dividing cancer cells. In doing so, it inevitably affects surrounding healthy cells.
But areas such as the bowel, lung and jaw seem to be more susceptible to long-term damage. The precise reason is not clear, although it is thought that the mucus which lines the bowel and the delicate sacs in the lung are extremely vulnerable.
Long-term damage can appear as fibrosis (an overgrowing of healthy cells as they go into overdrive to repair the radiotherapy damage) or necrosis (the death of the tissue, causing open holes or fistulas).
Radiotherapy can also damage nerves, reducing blood circulation or causing breathing difficulties, with side-effects often not appearing for several years after treatment.
When Alan Warren was diagnosed with rectal cancer four years ago, it was, understandably, very worrying. The taxi driver and father-of-two underwent chemotherapy, then radiotherapy, to shrink the tumour, before it was removed along with several inches of his bowel.
‘My oncologist said I would be back working within four months. Fours years on, I’m still unable to work,’ says Alan, 55.
During those years, Alan, from Christchurch, Dorset, has suffered unimaginable pain. He has also suffered the indignity of urine leaking out through his back passage after he developed an internal fistula 12cm long, running from the top of his bladder to what was left of his lower bowel.
An operation to close the fistula failed. After that, the only option was a permanent catheter.
‘My problems were all blamed on scar tissue from the original cancer surgery, so I was referred to a urologist for treatment.
‘By chance, Alan’s wife Jackie, a nurse, came across an article on radiotherapy damage. ‘My urologist reluctantly admitted that I probably did have it,’ says Alan.
In the UK treatment tends towards cutting out the afflicted area if necessary – which often results in more scar tissue and pain. But there are other options.
Jervoise Andreyev, a gastroenterologist at the Royal Marsden, London, uses anti-diarrhoea medication, pelvic exercises, antibiotics and dietary changes to treat the problem if it’s in the pelvis.
Meanwhile, Dr Delanian uses a combination of three drugs: vitamin E, pentoxifylline (for vascular and circulatory problems) and clodronate (bone disorders).
Her success rates are impressive, with research to back these up going back over a decade. After contacting the radiotherapy damage action group RAGE, Alan and Jackie found out about Dr Delanian, and in October last year they visited her in Paris. Thanks to treatment, by January 2008 Alan’s fistula was gone and he was healed.
Richard Wayman also saw Dr Delanian. Six months later, the hole in his face healed.
The leg weakness and tingling have stabilised, too.
But despite the fact that some UK doctors are quietly following her method, it is not a mainstream treatment, and many of her patients find that in the UK they are refused the drugs she prescribes.
In 2006, the Royal Marsden carried out a trial into Delanian’s treatment on breast cancer patients, but announced that it failed to show any significant improvement.
Paul Cornes says: ‘Newer radiation therapies such as intensity modulated radiation therapy (IMRT) and proton beam therapy deliver more accurate beams with significantly lesser side-effects.
‘Unfortunately, IMRT is not yet widely available in the UK, and proton beam therapy is considered too expensive for the NHS.’
Dr Delanian adds: ‘Radiation is a great tool, but can also be very dangerous. As a profession, we should try to find a way to minimise the risk and deal with the effects.’
Originally posted:
“This news story was resourced by the Oral Cancer Foundation, and vetted for appropriateness and accuracy.”

Leave A Comment
You must be logged in to post a comment.