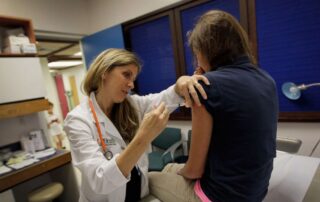
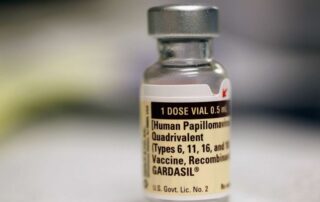
Most men benefit from initial and catch-up cancer prevention vaccination
Source: www.precisionvaccinations.com Author: Don Ward Hackett The Lancet Infectious Disease published the results from an extensive cancer prevention phase 3 study on November 12, 2021, supporting quadrivalent HPV vaccination in men, including catch-up vaccinations. The Gardasil quadrivalent human papillomavirus (HPV) vaccine was shown to prevent infections and lesions related to HPV6, 11, 16, and 18 in men aged 16–26 years. The researchers assessed the incidences of external genital warts related to HPV6 or 11 and external genital lesions and anal dysplasia associated with HPV6, 11, 16, or 18, over ten years of follow-up. The 3-year Base Study was an international, double-blind, randomized, placebo-controlled trial done at 71 sites in 18 countries. The Vaccination Period for the Base Study encompassed Day 1 through Month 7, during which time participants received qHPV vaccination at Day 1, Month 2, and Month 6. Follow-up for the Base Study encompassed Month 7 through Month 36. And the 7-year, open-label, long-term follow-up extension study was done at 46 centers in 16 countries. Between August 2010 and April 2017, 1,803 participants were enrolled in the long-term follow-up study, of whom 936 (827 heterosexual men and 109 MSM) were included in the early vaccination group and 867 (739 heterosexual men and 128 MSM) were included in the catch-up vaccination group. In early vaccine group participants during long-term follow-up compared with the placebo group in the Base Study, the incidence per 10 000 person-years of external genital warts related to HPV6 or 11 was 0·0 (95% CI 0·0–8·7) versus 137·3 [...]