Source: www.dailymail.co.uk
Author: Professor Lawrence Young
The seemingly unstoppable rise of throat and mouth cancers over the past two decades has left experts baffled and deeply concerned. These are truly horrible diseases. More than 15,000 new patients are diagnosed each year in Britain alone and almost 8,000 die from the most common type, cancer of the oesophagus. Two-thirds of sufferers are men. And those that survive are often left horrifically disfigured by aggressive radiotherapy and surgery. Most worryingly, numbers of new cases have doubled since 1989.
We used to think most oral and throat cancers – which also include laryngeal (voice box), tracheal (windpipe) and oropharyngeal (soft-palate) tumours – were due to a lifetime of smoking and heavy alcohol consumption, and only really occurred in old age. But as health messages hit home, numbers of smokers and drinkers dropped, fewer older men and women developed these cancers and a new group of patients – middle-class, middle-aged men who drank moderately and had never smoked – emerged. This was a surprise.
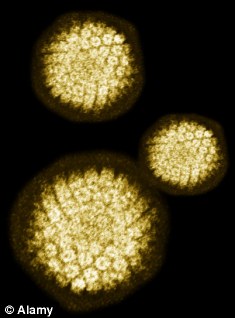
Threat: Small studies, in which oral cancer tumours were analysed, reveal a new culprit: the human papilloma virus
Small studies, in which tumours were analysed, indicated a new culprit: the human papilloma virus (HPV), the same virus that we knew was the cause of cervical cancer in women. For years there have been whisperings among oncologists that this could become one of the most significant cancer challenges of the 21st Century. And six weeks ago, evidence published by two American universities showed that these fears were becoming a reality.
Researchers found that about half of the male population carried some form of HPV; that every year there is a six per cent increase in carriers of HPV 16 and 18 – the deadliest forms of the virus; and that up to 64 per cent of head and neck cancers are likely to be caused by the virus.
HPV is an umbrella term for about 200 strains of virus. More than 40 types are transmitted through sexual contact. Some cause genital warts but most men and women who catch HPV never develop symptoms. I was involved in early screening studies that linked the virus to gynaecological cancers in women. Now I implore health chiefs to think seriously about vaccinating boys against HPV.
Since 2008, British girls between the ages of 12 and 13 been given the HPV vaccine Cervarix, which protects against HPV 16 and 18. Initially the programme was met with disdain – it was claimed that giving the vaccine would sexualise prepubescent girls. But it needs to be administered as early as possible before the onset of sexual activity as exposure to any strain of the virus renders the vaccine ineffective.
Some might think that vaccinating women is enough, but while teenage girls are supposed to be given the vaccine, there is no law to ensure every girl has it. Even optimistic figures put the amount of British girls having the jab at just 70 to 80 per cent. Furthermore, there has not been enough research about how HPV is transmitted from women to men – we still aren’t entirely sure if the vaccine stops a woman being able to carry the virus, even if she has been made immune to the effects of it.
Yes, sex has played a role in increasing the number of HPV-related cancers – it is incredibly difficult to transmit the virus without having sexual contact. Fifty years ago, sex before marriage was frowned upon and multiple partners were unusual. HPV can be transmitted from a woman to the mouth and throat of a man during oral sex. But this does not equate with promiscuity.
Carriers of HPV 16 or 18 can show no symptoms for many years before the cancer develops, so it is entirely possible to have just one sexual partner and contract the virus without even knowing it. The only thing that stands in the way of combating this deadly threat is funding. Currently the vaccine is not available for boys in the UK – neither on the NHS, nor privately. This, in my opinion, needs rethinking.
In the US, parents are already paying privately to get their sons vaccinated. The NHS is under huge financial stress and the announcement of £1billion in cuts turns a blanket vaccination for all British boys into a costs issue that must be debated. Adults cannot be vaccinated – for us, regular check-ups and limiting sexual partners are the only options. Once contracted, there is no way to get rid of HPV, although we hope to develop treatments. For the majority it won’t cause cancer.
More tests need to be done to fully understand how HPV is spread between men and women. And we need to demand, as parents, that our sons have the same right as their sisters in being protected against HPV.

Leave A Comment
You must be logged in to post a comment.