Source: www.drbicuspid.com
Author: Donna Domino, Features Editor
The James Graham Brown Cancer Center at the University of Louisville is among a growing number of facilities working to improve care for head and neck cancer (HNC) patients through collaborative care programs that bring together a spectrum of oncology specialists.
The center provides multidisciplinary treatment for HNC patients using novel techniques that decrease the debilitating side effects of radiation and chemotherapy. The clinic also conducts research and clinical trials with targeted therapies that aim to restore patients’ oral functions.
Kentucky has a higher rate of HNC than the U.S. average, which provides a large patient pool for the many clinical trials that the center conducts, according to Zafrulla Khan, DDS, MS, professor and director of maxillofacial/oncologic dentistry in the center’s HNC clinic.
“That’s what happens when you mix tobacco and bourbon,” Dr. Khan noted.
Intraoral radiation shields
Some of the center’s novel treatment techniques involve using intraoral radiation shields during brachytherapy radiotherapy procedures to prevent the tongue and nearby oral areas from getting irradiated while minimizing mucositis and xerostomia, Dr. Khan explained.

Intraoral radiation shields prevent the tongue and nearby oral areas from getting irradiated while minimizing mucositis and xerostomia
“We put catheters right into tumors so they can deliver the radiotherapy in the mouth with high-density therapy machines rather than doing an external beam,” he said.
The clinic also uses a surgical obturator, a prosthetic device that enables patients to speak and swallow following surgery for maxillary sinus cancer. The maxillectomy procedure removes bones and tissue in the hard palate of the mouth, so when patients try to eat, the food can come through the nose, sinuses, and even into the lungs.
The device is similar to a denture or partial and includes a bulb that fills the opening in the roof of the mouth and part of the soft palate if it’s missing.
“It’s like a denture with a hump,” Dr. Khan explained. “It might be crude and simplistic but it gives patients the ability to eat orally and speak. That’s two major functions that are restored.”
The novel approaches are among the advantages of having a multidisciplinary team that includes maxillofacial oncologists, he noted.
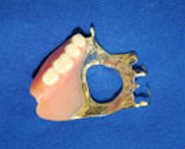
The surgical obturator is a prosthetic device that enables patients to speak and swallow following surgery for maxillary sinus cancer.
Previously, surgeons consulted with specialists individually, Dr. Khan said. Weekly meetings with the center’s specialists include an HNC pathologist, radiation oncologist, medical oncologist, otolaryngology surgeon, ear nose and throat specialist and Dr. Khan, who is a dental oncologist/maxillofacial prosthodontist.
Multidisciplinary approach
The center also has a palliative care physician for pain management, nurse study coordinator for the clinical trials, speech pathologist, and social worker for indigent patient needs such as transportation.
“We meet Friday mornings and everybody gets their two cents in,” Dr. Khan said. “What if we do this or that? So the overall plan is much better simply because everyone has input before you present treatment options to the patient. You’re not second guessing what the radiologist, medical oncologist or surgeon is thinking because they’re all at the table. I think it’s the only real way to treat cancer nowadays.”
One of his most interesting and unusual cases involved maxillary prosthodontics for a bodyguard whose face had to be largely replaced after he developed a fungal infection in his maxillary sinus. “He was a diabetic on steroids, and he ignored the infection too long,” Dr. Khan told DrBicuspid.com.
A specialty team including plastic, microvascular and maxillofacial oral surgeons performed a bilateral orbital exenteration (removing the contents of the eye socket), a maxillectomy (removal of the bones along the palatal fissure that forms the upper jaw) and also removed his upper lip.
“His face was pretty much carved off,” Dr. Khan said. “Everything was removed up to the base of his skull. We redid his face completely.”
The man’s eyes were replaced with prosthetic eyes and his upper palate was reconstructed with free flaps grafts from his fibula.
Afterward, his face was “reasonably acceptable,” Dr. Khan said. But sadly, he became sedentary after he lost his vision and died about seven years later when he was only in his 40s.
Improving quality of life
The first line of therapy for HNC patients is now shifting more toward radiation and chemotherapy, Dr. Khan observed.
“When I first started it was surgery followed by radiation because it was close to a positive margin and there might be nodal involvement,” he recalled. In fact, the center’s surgical rate for HNC dropped from 43% in 2004 to 23% in 2006.
“It makes a lot of sense because you can always do surgery later,” he noted.
All HNC patients must get a dental clearance and any needed extractions before radiation therapy to avoid complications later. “It’s essential and minimizes the side effects that you used to see,” Dr. Khan explained. “But there’s no escaping xerostomia and mucositis because that’s the nature of the therapy.”
HNC cases are hugely expensive, he noted. An average seven-day treatment course costs between $40,000 to $60,000 just for radiation therapy.
Some 40% of the patients are indigent, but their costs are covered because the center is a university-based hospital, he noted. “We never turn down patients because of their inability to pay.”
For Dr. Khan, the main priority is improving the lives of his patients.
“Quality of life is so critical,” he said. “I don’t care who the patient is, when they have a cancer diagnosis they’re devastated. Even if it’s a late diagnosis, we as dentists can make their quality of life a lot better.”

Leave A Comment
You must be logged in to post a comment.